TEST & PROCEDURES
Our team of physicians are trained in all aspects of gastrointestinal disorders.
After an initial gastroenterology consultation, our doctors may perform procedures including:

The U.S. Preventive Services Task Force recommends that adults age 50 to 75 be screened for colorectal cancer. The decision to be screened after age 75 should be made on an individual basis. Individuals at an increased risk of getting colorectal cancer should talk to their doctor at DDM about when to begin screening, which test is right for them, and how often to get tested. Several screening tests can be used to find polyps or colorectal cancer.

A colonoscopy/polypectomy may be recommended as a screening test for colorectal cancer. Colorectal cancer is the third leading cause of cancer deaths in the United States. Annually, approximately 150,000 new cases of colorectal cancer are diagnosed in the United States and 50,000 people die from the disease. It has been estimated that increased awareness and screening would save at least 30,000 lives each year. A colonoscopy lets your doctor examine the lining of your large intestine (colon) for abnormalities by slowly advancing a thin flexible tube into your colon. This instrument, called a colonoscope, enables your doctor to visualize images of your colon on a video monitor to detect abnormalities.
To prepare for a colonoscopy, your doctor will tell you what dietary restrictions to follow and what cleansing routine to use. In general, the preparation consists of limiting your diet to clear liquids the day before and consuming either a large volume of a special cleansing solution or special oral laxatives. The colon must be completely clean for the procedure to be accurate and comprehensive, so be sure to follow your doctor’s instructions carefully. A colonoscopy is well-tolerated and rarely causes much pain. You might feel pressure, bloating or cramping during the procedure. Typically, your doctor will give you a sedative or painkiller to help you relax and better tolerate any discomfort. You will lie on your side or back while your doctor slowly advances a colonoscope along your large intestine to examine the lining. Your doctor will examine the lining again as he or she slowly withdraws the colonoscope. The procedure itself usually takes less than 45 minutes, although you should plan on two to three hours for waiting, preparation and recovery. In some cases, the doctor cannot pass the colonoscope through the entire colon to where it meets the small intestine. Your doctor will advise you whether any additional testing is necessary.
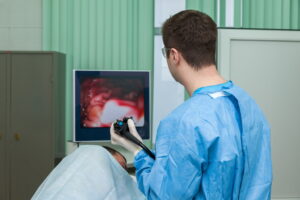
Gastroscopy (Upper Endoscopy/EGD)
An upper endoscopy helps your doctor evaluate symptoms of upper abdominal pain, nausea, vomiting or difficulty swallowing by allowing your doctor to examine the lining of the upper part of your gastrointestinal tract, which includes the esophagus, stomach and duodenum (the first portion of the small intestine). Your doctor will use a thin, flexible tube called an endoscope, which has its own lens and light source, and will view the images on a video monitor. To prepare for an upper endoscopy, an empty stomach allows for the best and safest examination, so you should have nothing to eat or drink, including water, for approximately six hours before the examination. Your doctor will tell you when you should start fasting as the timing can vary.
At the start of the upper endoscopy, the doctor might start by spraying your throat with a local anesthetic or by giving you a sedative to help you relax. You’ll then lie on your side, and your doctor will pass the endoscope through your mouth and into the esophagus, stomach and duodenum. The endoscope doesn’t interfere with your breathing. Most patients consider the test only slightly uncomfortable, and many patients fall asleep during the procedure. An upper endoscopy is also referred to as a EGD or Gastrocopy.
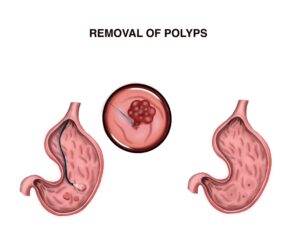
Stomach polyps — also called gastric polyps — are masses of cells that form on the lining inside your stomach. These polyps are rare and usually don’t cause any signs or symptoms. Stomach polyps are most often discovered when your doctor is examining you for some other reason.
Most stomach polyps don’t become cancerous. But certain types can increase your risk of stomach cancer in the future. Depending on the type of stomach polyp you have, treatment might involve removing the polyp or monitoring it for changes.

In people who have cirrhosis, high pressure in the veins that carry blood from the intestines to the liver (portal hypertension) causes many problems. Variceal bleeding—bleeding from enlarged veins (varices) in the digestive tract—is an extremely serious complication of portal hypertension. For people who have advanced cirrhosis and varices, especially in the esophagus, the risk of variceal bleeding is high. After varices have bled the first time, there is a high risk of bleeding again. The chance of bleeding again is highest right after the first bleed stops. Then the chance of bleeding again gradually goes down over the next several weeks. If varices are not treated, bleeding can lead to death.
During variceal banding, a doctor uses an endoscope to place an elastic ring that looks like a rubber band around an enlarged vein. Banding the vein in this manner will cut off blood flow through the vein. It may be difficult to use this procedure while someone is actively bleeding, because the device used to place the bands obscures the doctor’s vision.
Variceal banding has been shown to be as effective as sclerotherapy in treating episodes of bleeding, and it has fewer complications. Variceal banding is often done several times to control the varices and prevent bleeding. For example, banding might be repeated every 2 to 4 weeks for 3 to 4 sessions. Your doctor will monitor (check) the varices every 3 to 12 months after that for the rest of your life.

Hemorrhoidal banding is a non-surgical method for treating and removing hemorrhoids. Hemorrhoids are swollen vessels in the lower rectum and anus caused by increased pressure or straining. While not life threatening, hemorrhoids can cause bleeding, burning or discomfort.
For decades, chronic hemorrhoid sufferers resorted to surgery for relief. Today, a procedure called the CRH-O’Regan Disposable Hemorrhoid Banding System has all but eliminated the need for surgery and allows patients to be treated quickly and resume normal activity with very little discomfort.
Most patients with office jobs find they can return to work the same day. The O’Regan method uses a small rubber band to strangle the base of the swollen vein, which cuts off the blood supply to the hemorrhoid. This causes the banded tissue to shrink and fall off along with the rubber band. Typically, this happens within a few days after your appointment during a routine trip to the toilet, and you may not even notice when this happens. The treatment itself takes less than five minutes and can be performed in one of our offices or endoscopy centers.
Our physicians trained in this procedure tend to avoid doing more than one treatment per visit. Subsequently, some patients who have multiple hemorrhoids may require two or three treatments which are scheduled a few weeks apart.
The band placement is relatively painless due to this refined technique and it does not require anesthesia or other numbing agents. You may experience a dull ache or sense of fullness in the rectum within the first 24 hours, but this can generally be relieved by over-the-counter pain medication.
